My lab develops high-resolution optical imaging technology for biomedical applications. We aim to help bring affordable microscopic imaging to the point-of-care, maximising the benefits of technology for patients. We try to use computational imaging techniques to achieve performance similar to large and expensive bench-top microscopes, but in low-cost, small form-factor devices.
My lab develops high-resolution optical imaging technology for biomedical applications. We aim to help bring affordable microscopic imaging to the point-of-care, maximising the benefits of technology for patients. We try to use computational imaging techniques to achieve performance similar to large and expensive bench-top microscopes, but in low-cost, small form-factor devices.Contacts: Physics & Astronomy, Ingram Building, University of Kent, CT27NH. Email: m.r.hughes@kent.ac.uk
More details on my current research are below. For information on my background and university roles, including teaching on the physics programme, and a list of publications, see my school profile page. Some software developed in the lab is also available for download, or you can look at current projects on Github. Various other things, including lecture notes, are available here. I occasionally write a blog, Photons For Life.
Opportunities
I will advertise funded positions when available, and I can offer projects for Masters or PhD students who are seeking funding through scholarship schemes or who are self funded. There are usually some EPSRC studentships available at the University, advertised around January, as well as various other scholarships. Please contact me if you are interested and would like some advice. Some example projects, adaptable for PhD or MSc degrees, are below, but I’m happy to discuss other possibilities, please get in touch.
- Imaging through ultrathin fibres
- Advanced imaging through fibre bundles
- Compact holographic microscopy for microfluidics
- A low-cost medical imaging device
Summer internships can also be offered for current undergraduate students, an example report from a previous intern can be read here.
Research
We work on hardware and software for imaging and microscopy. Most of our software is open source on Github.
Endoscopic Microscopy
Endoscopic microscopes (or endomicroscopes) allow us to image tissue in vivo, at high resolution and in real time, potentially reducing the need for invasive biopsy. We work on the development of new techniques for fibre bundle based endomicroscopes, enhancing the resolution and optical strengthening power, and on making devices lower cost and more accessible. I begin this work as a postdoc at Imperial College, where I developed a technique for achieving very high frame rate optically-sectioned fluorescence endomicroscopy [Paper1, Paper2]) and worked on a study for the Bill and Melinda Gates Foundation on potential applications in gut dysfunction [Paper]. At Kent we have developed a new approach which allows a computational sectioning technique, structured illumination endomicroscopy, to be used with a moving probe [Paper] and made further improvements to line-scanning endomicroscopy [Paper]. We developed and maintain PyFibreBundle, a Python package for imaging with bundles [Paper] and providing state-of-the-art performance in image reconstruction. I also have an interest in white light microscopy via fibre bundles [Paper1, Paper2] .
Fibre bundle endomicroscope inside an endoscope
Optical Coherence Tomography (OCT)
Optical Coherence Tomography (OCT) is a high-resolution biomedical imaging technique, able to acquire images up to around 1 mm below the tissue surface. It is particularly important in retinal imaging, and is now available in High Street opticians. Kent is a well-known for it’s OCT research, and the Applied Optics Group has been a leader in the field for many years. I am particularly interested in endoscopic, miniaturised and low-cost OCT, particularly approaches suitable for new medical applications outside of opthalmology and cardiology. I am co-investigator on grants on endoscopic OCT (EPSRC), applications of OCT in agriculture (BBSRC), and OCT imaging and sensing for robotic opthalmic surgery (NIHR), and I co-supervise two PhD students in this area. I also recently completed two BBSRC and MRC Impact Accelerator grants to develop a low-cost OCT, and have collaborated on projects relating to speckle reduction in OCT [Paper].

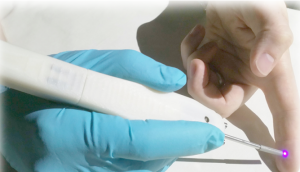
The OCT Pen, developed in my lab.
Holographic Microscopy
Inline Holographic microscopy is a type of computational microscopy which is lensless – images are synthesised from holograms. This has some major advantages in terms of building a small, compact, and low-cost microscope. It also allows us to numerically refocus the images: a single hologram can subsequently be focused in software to any position we wish.
We have recently developed a new method for building miniature holographic microscopes using fibre bundles [Paper], and with funding from the Royal Society we are now building further prototypes, working on improved resolution [Paper] and depth range [Proceeedings], and exploring potential applications.
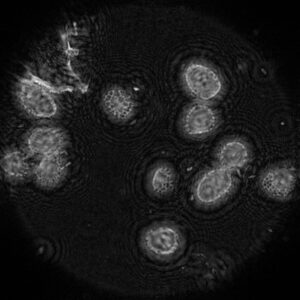
Lillium anther on a slide imaged through fibre bundle inline holographic microscopy, using resolution enhancement.
Microscope in a Needle
To build a useful needle microscope, able to image deep inside tissue with minimal invasiveness, we need to make a high-resolution image conduit which is less than a few hundred microns in diameter. With previous funding from EPSRC, we are exploring ways of transmitting images through single-core multimode fibres by exploiting interference between the fibre modes [Paper]. Read More.
Robotic Microscopy and Imaging
While working at the Hamlyn Centre for Robotic Surgery at Imperial College London with Prof Guang-Zhong Yang I developed an interest in robot-guided imaging probes [Paper1, Paper2, Paper3, Paper4, Paper5]. I later collaborated with Prof Adrian Podoleanu at Kent and a team from the Hamlyn Centre on the REBOT Project (Robotic Endobronchial Optical Tomography) to develop robot-guided imaging probes [Paper], particularly for the lung. We are now working with King’s College London and Moorfields Eye Hospital to integrate sensing and imaging probes into robotic opthalmic surgery (Press Release).
Robotic OCT and fluorescence imaging, developed in collaboration with Hamlyn Centre, Imperial College London.
Outreach
I am keen to help share my excitement about physics, optics and biomedical imaging. In addition to Applied Optics Group outreach activities I can give talks and hands-on demos to schools (secondary level or above) or other interested groups. Two examples of talks are below, these can be customised for different audiences. Please contact me for more information:
Physics and Light in Medicine: From Pulse Oximeters to Robotic Surgery
Physics underpins much of our modern world, and medical technology is no exception. For those interested in the physical world, but also in applying this knowledge to real-world problems, the medical applications of physics can provide a fascinating and rewarding career. This talk provides an overview of how physics lies behind different diagnostic and therapeutics techniques used in healthcare, from pulse oximeters to external beam radiotherapy. We will focus particularly on some emerging technologies which use light imaging to provide new insight into disease, and which in the future may be used to guide advanced procedures such as robotic surgery.
A Very Brief Introduction to Einstein’s Theory of Special Relativity
In 1905, Albert Einstein published his paper “On the Electrodynamics of Moving Bodies”, marking the beginning of the era of modern physics. This theory tells us that space and time are intimately related, and that there is an ultimate speed limit in the Universe – the speed of light, or ‘c’. Accounting for this speed limit leads us to some seemingly bizarre conclusions: that time passes differently for different observers, that two observers cannot agree on whether two events are simultaneous or not, and ultimately that there must be a fundamental relationship between mass and energy, encapsulated in the famous equation E = mc2. This talk explores some of the key ideas behind special relativity, using the simple maths of algebra and trigonometry to explain one of the most exciting scientific ideas of the twentieth century.